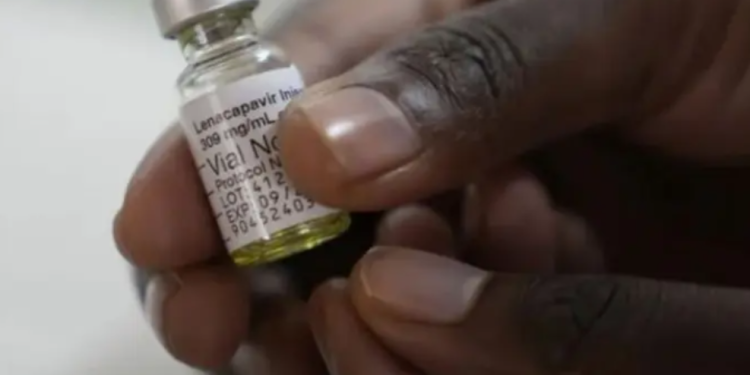A drug already in use for treating certain HIV infections has now received approval from the U.S. Food and Drug Administration, FDA, for use in preventing HIV.
Gilead Sciences, the drug’s manufacturer, announced that Lenacapavir administered as a twice-yearly injection has been approved for HIV prevention under the brand name Yeztugo. Clinical trials found the drug to dramatically reduce the risk of HIV infection, offering near-total protection and outperforming currently available options for pre-exposure prophylaxis, PrEP.
PrEP therapies have long been used to prevent HIV infections. In the United States, this typically involves taking a daily pill like Truvada or receiving bi-monthly injections like Apretude. Yeztugo now introduces a groundbreaking new option as the first and only twice-a-year HIV prevention shot.
READ ALSO: NACA launches initiative to make Taraba HIV-free
“Yeztugo could be the transformative PrEP option we’ve been waiting for,” said Dr. Carlos del Rio, professor of medicine at Emory University and co-director of its Center for AIDS Research. “This new option could help address barriers like stigma and adherence that patients often face with daily or more frequent PrEP regimens.”
Dr. Jared Baeten, senior vice president at Gilead, emphasized how Lenacapavir works: “By having this medicine in your body, if you encounter HIV, it blocks the virus from taking hold.”
HIV, primarily spread through unprotected sex or sharing needles, attacks the immune system and can lead to AIDS without treatment. Although new infection rates in the U.S. have dropped, an estimated 1.2 million Americans live with HIV, and about 13% are unaware of their status.
Clinical Breakthrough
The PURPOSE 2 trial revealed that just two Lenacapavir injections per year reduced HIV infection risk by 96%. Another trial, PURPOSE 1, showed 100% efficacy in women.
“Lenacapavir offers a private, discreet option for many peopleVjust set it and forget it,” said Baeten. “This could make HIV prevention far more workable for people’s lives.”
Ian Haddock, who participated in the PURPOSE 2 trial, shared his story. As a teen in rural Texas, he faced stigma when coming out. “The first thing my family said was, ‘You’re going to get AIDS,’” he recalled. Now 37, Haddock doesn’t have HIV and leads the nonprofit Normal Anomaly Initiative. He had been on daily PrEP since 2015 but often forgot doses or experienced side effects. Since joining the trial in 2024, Haddock has experienced only minor injection site irritation and plans to continue with Lenacapavir.
Despite PrEP’s availability since 2012, many remain unaware or misinformed. “People often confuse PrEP with having HIV or being promiscuous,” Haddock said. “Lenacapavir opens a completely new chapter.”
A Milestone in HIV Prevention
Data from Gilead’s trials show that 99.9% of Lenacapavir recipients did not contract HIV. Out of 2,180 participants, only two became infected, making it 89% more effective than Truvada. The trial included cisgender men, transgender people, and nonbinary individuals aged 16 and older. Some pregnant participants continued treatment safely.
“This is a milestone in our decades-long fight against HIV,” said Gilead CEO Daniel O’Day. “With only two injections a year, Lenacapavir is a scientific breakthrough that could protect millions.”
Cost and Availability
Gilead says patients can start asking providers about Yeztugo within two days, though it might take up to two months to receive the first dose, depending on insurance coverage.
Pricing for Lenacapavir as a PrEP drug has not been finalized. For HIV treatment, the drug currently costs up to $45,000 per year without insurance. However, research suggests it could be mass-produced for as little as $40–$93 per year if generic competition and voluntary licensing are adopted.
Lenacapavir follows Apretude, which was approved in 2021 as the first injectable PrEP. Experts hope such tools can end HIV transmission within a generation.
“Strong prevention, along with testing and treatment, can end this epidemic,” said Baeten. “This generation has the chance to end HIV and the next one might not even have to think about it.”
Policy Concerns
Despite this breakthrough, the Trump administration’s 2026 budget proposal threatens to slash over $1.5 billion in HIV prevention, research, and surveillance programs.
“Now is not the time to pull the rug out from under HIV prevention,” said Carl Schmid, executive director of the HIV+Hepatitis Policy Institute. “Cutting CDC programs will only raise infection rates and healthcare costs. Congress must act to stop these cuts.”
NEWSEXPRESSNG
—